Dupuytren's Contracture
What is Dupuytrens Contracture?
Dupuytren's contracture is a progressive thickening and tightening of tissue in the palm of the hand and fingers. This condition typically causes the ring and little fingers to bend into the palm.. Dupuytren's is not a serious condition but it cannot be cured and there is a significant chance of it recurring. There are a number of factors which can predispose patients developing Dupuytren's disease. It tends to run in families and can be associated with diabetes, excess alcohol intake and epilepsy. In the vast majority of patients we do not know why they develop the disease.
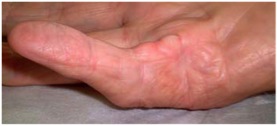
Thickening and cord like structures develop gradually in the palm and extend into the fingers causing the fingers to roll up into the palm. In the initial stages nodules develop and can be tender but this usually settles.
What is the Non operative treatment?
Splints can help to prevent the contracture from developing but these are uncomfortable and poorly tolerated.
Injections of enzymes are an exciting new development which has been proven to work in a large trial which has recently been completed. click here for more information
It is possible to release the cords with needleing through the skin; we can only offer this treatment in certain patients with a single contracture limited to the palm. It is performed in outpatients and must be splinted for 3 months. Recurrence is more common than with surgery.
What is the operative treatment?
The hand has a unique fascia which is like a canvas under the skin.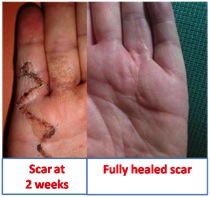 Normally it acts to toughen the skin allowing us to twist and grip things without injury. When thickened and contracted the fascia can be removed with an operation called a fasciectomy. The surgery will correct the deformity of the fingers if they have not progressed too far. A zigzag cut is used as a straight incision would contract and the Dupuytrens contracture would recur early. The scar looks extensive at first site after the operation but almost completely disappears over a few weeks to months.
Normally it acts to toughen the skin allowing us to twist and grip things without injury. When thickened and contracted the fascia can be removed with an operation called a fasciectomy. The surgery will correct the deformity of the fingers if they have not progressed too far. A zigzag cut is used as a straight incision would contract and the Dupuytrens contracture would recur early. The scar looks extensive at first site after the operation but almost completely disappears over a few weeks to months. If the Dupuytrens has recurred or the Dupuytrens tissue extends all the way into the skin it may be necessary to remove the skin altogether and replace it with skin from the forearm. This is called a dermofasciectomy.
What can I expect during recovery?
Local anaesthetic will be injected into the wound at the end of the operation. This area and the fingers will remain numb for up to six hours after surgery. Before the effect wears off, you should take painkillers which have been prescribed on a regular basis. Your hand will initially be placed in either a bulky dressing, or a plaster splint.Swelling causes stiffness and pain which is made worse by hanging the arm down at your side or resting it on your lap. Swelling is best prevented by keeping the hand above the level of the heart for the first 48 hours.
You will be seen within a few days by the Hand Therapist. The dressings will be removed and the wound will be checked. You will be given advice and exercises to start immediately. Hand elevation remains important to prevent swelling and stiffness of the fingers. Please remember not to walk with your hand dangling, or sit with your hand held in your lap. If the hand becomes red, hot and very swollen you must go to your GP or the Accident and Emergency Department
At this time a Hand Therapist appointment will be made for the following week to check your exercises.
Your stitches are absorbable so they will not need to be removed. If the wound is healing well, you may be referred to the Occupational Therapist for a splint to be worn at night. The splint is to be worn for approximately 12 weeks to keep the fingers straight. During the day, the hand should be exercised and you should perform normal activities.
At this stage it is safe to get the hand wet. The wound and the surrounding skin often become very dry and will be more comfortable if a moisturiser is applied, including on the wound itself. Initially the scar will be thickened and tender to touch. This must be massaged firmly with a moisturising cream to reduce sensitivity and swelling.
After two weeks you can usually drive a car as long as you are comfortable and have regained full finger movements. Timing of your return to work varies with your occupation and this should be discussed with your therapist.
What can I expect from my surgery?
- More than 95% of patients are happy with the result. However complications can occur.
- Recurrence over a life time is almost inevitable; however, most patients have a long lasting result that they are happy with.
- Incomplete correction of the contraction, the surgery fails to straighten the finger. This is particularly common when there has been a longstanding contracture of more than 90 degrees.
- Injury to the blood vessels and nerves to the finger (very much less than 1%) may leave one side of the finger numb. If this occurs the wound should be explored and if injured, the nerve repaired.
- When skin grafts are used (dermofasciectomy), a small number fail to heal.
- Infection (Less than 1%), scar pain and Numbness.
- Reflex Sympathetic Dystrophy This is a rare complication but is unpleasant if it occurs. The hand goes into shock; the fingers become shiny, stiff and very painful to even light touch . It resolves on its own with physiotherapy to help prevent the stiffness. Very rarely, severe cases can continue for many months and injections by the pain team may be needed.



